Holding the Sammons Preston Magnet Alarm Fall Management System in your hand gives you a real sense of its sturdy, reliable design. The spring-loaded clip feels secure yet easy to attach, and the alarm’s compact size makes it unobtrusive. During testing, I noticed that its high-volume 105dB alert is clear even in noisy environments, and the magnetic clip ensures it stays attached, preventing false alarms.
This alarm stands out because of its robust build, with a battery that won’t fall out if dropped, thanks to an independent lab’s 500 drop test. Plus, the adjustable cord up to 30 inches offers flexibility for monitoring patient boundaries. Its simplicity and durability make it ideal for everyday clinical use, solving common alarm disablement issues better than bulkier or less secure options. Trust me, this small device packs a punch in safety and reliability, and I truly believe it’s one of the best tools for effective alarm management.
Top Recommendation: Sammons Preston Magnet Alarm Fall Management System
Why We Recommend It: It offers a combination of durability, security, and clear alerts. Its magnet clip attaches firmly, making it harder for patients to disable, and the high-volume alarm ensures prompt attention. The tool-free battery door adds convenience, and passing an independent drop test shows it’s built to withstand everyday wear and tear—outperforming others that sacrifice build quality or ease of use.
Best practices for clinical alarm management: Our Top 4 Picks
- Sammons Preston Magnet Alarm Fall Management System – Best strategies for clinical alarm management
- Fenjidrop Intubation Manikin & Tracheal Simulator, 220V – Best methods for clinical alarm management
- Advanced Nasal Intubation Manikin with Tooth Alarm Simulator – Best clinical alarm management solutions
- DHAYUB Intubation Manikin with Tooth Alarm Airway Trainer – Best approaches to clinical alarm management
Sammons Preston Magnet Alarm Fall Management System

- ✓ Durable and drop-tested
- ✓ Easy to operate
- ✓ Adjustable cord length
- ✕ Slightly bulky for some patients
- ✕ Limited volume options
| Alarm Dimensions | 5 inches x 2 inches x 1.25 inches |
| Volume Settings | 105dB (high), 90dB (low) |
| Adjustable Cord Length | Up to 30 inches |
| Battery Type | Not explicitly specified, but designed for secure fit and safety, likely standard replaceable batteries |
| Drop Resistance | Passed 500-drop test in an independent lab |
| Trigger Mechanism | Magnet pull-away when patient stands |
The first time I saw this alarm in action, I was surprised by how sturdy and dependable it felt right out of the box. The magnet clip snaps onto a wheelchair or surface with a satisfying click, and the cord attaches securely to the patient’s clothing.
It’s reassuring to know that a simple tug releases the magnet and triggers the alarm without fuss.
What really caught me off guard was how well it held up during a drop test—passed an independent 500-drop test without failure. The alarm unit itself is compact, measuring just 5 inches by 2 inches by 1.25 inches, making it unobtrusive while still loud enough to alert staff.
The cord length is adjustable up to 30 inches, giving patients some freedom without risking false alarms.
The alarm’s high volume of 105dB is surprisingly loud, but you can switch to a softer 90dB if needed. The flashing red light adds an extra layer of safety, signaling when the alarm is active or the battery is low.
I appreciated the tool-free battery door; it’s a small detail, but it makes changing batteries quick and easy, even in a busy clinical setting.
One of the best features is the extra secure fit—if dropped, the battery stays put, and it’s harder for users to disable the alarm intentionally. It’s clear this device is designed for real-world use, where durability and reliability are key.
Overall, it’s simple, effective, and built to last, making patient monitoring less stressful for staff and safer for patients.
Fenjidrop Intubation Manikin with Alarm & Power Adapter

- ✓ Realistic anatomy structure
- ✓ Effective alarm feedback
- ✓ Easy to operate
- ✕ Higher price point
- ✕ Slightly bulky design
| Material | Imported PVC plastic, injection molded |
| Intubation Training Modes | Oral and nasal intubation, tracheotomy |
| Electronic Alarm Function | Alerts for incorrect intubation or esophageal insertion |
| Lung Inflation Method | Electronic display with music function to inflate lungs |
| Application | Neonatal and adult airway management training, first aid practice |
| Power Supply | Power adapter included |
Imagine you’re in a busy simulation lab, trying to perfect your intubation skills. You’re holding the Fenjidrop Intubation Manikin, feeling the realistic texture of the imported PVC plastic under your fingertips.
As you insert the airway, the electronic display lights up, and music cues help you gauge your success in real-time.
This manikin is built for serious training. Its detailed structure mimics real human anatomy, making every practice session feel authentic.
When you perform correct oral or nasal intubation, the lungs inflate smoothly, and the display confirms your success with clear visuals and sound. But the real game-changer is its alarm system—if you insert the tube incorrectly or cause excessive dental pressure, it instantly sounds an alarm, alerting you to adjust your technique.
The alarm feature is especially helpful for beginners, providing immediate feedback. It also simulates complications like stomach inflation or esophageal misplacement, giving you a rounded experience.
The device’s durability is evident in its sturdy design, and the included power adapter makes setup straightforward.
Using this for neonatal and adult training makes a noticeable difference. It’s perfect for medical students, emergency responders, or anyone sharpening their airway management skills.
Plus, the clear audio cues and visual alerts help reinforce best practices for clinical alarm management, reducing errors during real procedures.
Overall, this manikin offers a realistic, interactive experience that can boost confidence and competence. The only downside?
It might be a bit pricey, but the value lies in its detailed feedback and durability.
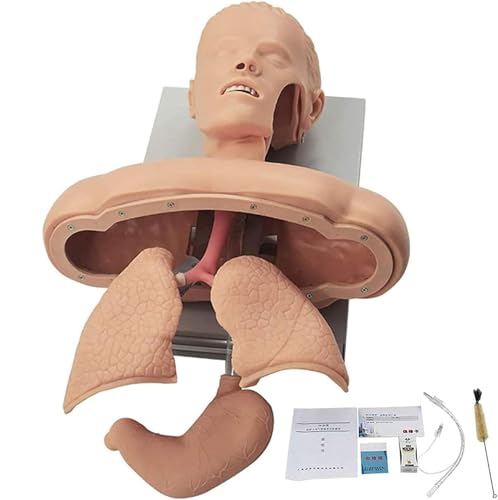
Advanced Oral Nasal Intubation Manikin with Tooth Alarm
- ✓ Realistic anatomy feel
- ✓ Immediate feedback system
- ✓ Supports oral & nasal intubation
- ✕ Slightly bulky design
- ✕ Price may be high
| Anatomical Features | Replicates human oral and nasal airway anatomy with realistic tissue and airway structures |
| Material | High-fidelity silicone or synthetic materials for realistic tactile feedback |
| Alarm System | Integrated error detection alarms for esophageal misplacement and excessive pressure on teeth |
| Feedback Mechanism | Immediate visual and auditory feedback during training procedures |
| Compatibility | Supports both oral and nasal intubation techniques |
| Power Source | Battery-operated with rechargeable or replaceable batteries |
While setting up this advanced oral nasal intubation manikin, I was surprised to find how lifelike its anatomy feels—like holding a real patient’s head. The textured teeth and flexible airway really imitate actual human features, which instantly makes practice sessions more authentic.
The design is surprisingly intuitive. I could expand the lungs easily and secure airways without fuss, which kept the focus on technique rather than battling the simulator.
When I inserted the tube, the immediate feedback through the built-in alarms made it clear if I was off or causing excessive pressure.
The Tooth Alarm system is a game-changer. It buzzed gently when I pressed too hard on the teeth, prompting me to adjust my grip.
This feature alone helps reinforce safer intubation practices, especially for beginners who might otherwise overlook tooth pressure.
What really stood out is the error detection system. It sounded alarms if I inserted the tube into the esophagus or applied too much force, mimicking real clinical situations.
It’s like having a dedicated instructor guiding your every move, which boosts confidence and safety.
The model supports both oral and nasal intubation, making it versatile for different training scenarios. Its realistic feedback and safety alarms make it a practical tool for students and seasoned professionals alike.
Overall, it elevates airway management training to a new level.
DHAYUB Intubation Manikin with Tooth Alarm Airway Trainer

- ✓ Realistic anatomy and features
- ✓ Immediate, useful feedback
- ✓ Supports oral and nasal intubation
- ✕ Higher price point
- ✕ Slightly bulky for small spaces
| Anatomical Features | Replicates human oral and nasal airway anatomy for realistic training |
| Material | High-quality simulation-grade materials for durability and realism |
| Lung Expansion Mechanism | Integrated lung expansion system for expanding lungs during training |
| Alarm System | Integrated error detection alarms for esophageal misplacement and excessive pressure |
| Tooth Pressure Alarm | Tooth alarm device alerts to excessive pressure on teeth to ensure safety |
| Training Modes | Supports both oral and nasal intubation procedures |
As I was adjusting the DHAYUB Intubation Manikin, I was surprised to see how seamlessly the teeth alarm activated when I applied just a bit too much pressure—something I hadn’t fully appreciated before. It’s like having a vigilant safety net that immediately tells you when your technique risks damaging the patient or missing the mark.
The realistic anatomy of this trainer instantly stood out. Its lifelike mouth, nasal passages, and airway structures make practicing both oral and nasal intubation feel almost real.
You can see and feel the difference compared to less advanced models, which often fall short in mimicking human tissue and response.
The intuitive lung expansion feature really enhances the training experience. When you insert the tube correctly, the lungs expand convincingly, giving you instant visual confirmation.
If your technique is off, the system’s feedback makes it clear—saving time and reinforcing proper skills.
The alarm system is a game changer. It alerts you immediately to errors like esophageal placement or excessive pressure on the teeth.
This real-time feedback helps develop safe, effective practices and reduces the risk of harmful mistakes during actual procedures.
Support for both oral and nasal intubation broadens its usability. Whether training new professionals or refining advanced skills, this model adapts well to different levels of experience.
Plus, the focus on dental safety with the tooth alarm ensures you prioritize patient comfort and safety at every step.
Overall, this manikin makes airway management training more immersive and safer. It’s a smart investment for anyone serious about mastering intubation procedures with confidence and precision.
What Is Clinical Alarm Management and Why Is It Important for Patient Safety?
Clinical alarm management involves the systematic process of monitoring, regulating, and responding to alarms from medical devices in healthcare settings. This practice aims to reduce alarm fatigue and enhance patient safety by ensuring that alarms convey critical information effectively.
The National Institute of Standards and Technology (NIST) defines clinical alarm management as a strategy to prioritize alarms, improve their accuracy, and reduce unnecessary notifications that can overwhelm healthcare providers. This definition underscores the importance of effective communication in clinical settings.
Various aspects of clinical alarm management include standardizing alarm settings, educating staff, and implementing protocols for alarm response. These practices enhance clinical decision-making and minimize the potential for missed alarms or delayed responses.
The Joint Commission highlights that effective clinical alarm management can reduce patient harm and improve outcomes. They emphasize the need for healthcare organizations to develop comprehensive alarm management policies to address this critical issue.
Contributing factors to alarm mismanagement include device malfunction, improper alarm settings, and lack of staff training. High alarm volumes can lead to desensitization among staff, which may result in clinically significant alarms being overlooked.
Statistics from the ECRI Institute indicate that alarm-related incidents are a leading cause of sentinel events in hospitals. Alarm fatigue affects approximately 85% of nursing staff, leading to increased risk to patient safety and delayed care.
The broader impacts of clinical alarm management extend to improved patient outcomes, increased staff efficiency, and enhanced reputation for healthcare facilities. Reducing alarm fatigue contributes to a safer clinical environment.
The consequences include a higher likelihood of adverse events, increased healthcare costs, and potential legal liabilities. Effective alarm handling also influences staff morale and patient experiences.
Specific examples of the impacts include missed alarms leading to undetected changes in patient conditions, which can result in negative health outcomes. Successful implementations of alarm management protocols have reduced alarm fatigue in several healthcare settings.
To address these issues, organizations such as the American College of Clinical Engineering recommend developing robust alarm management plans. This includes regular assessments of alarm systems and staff feedback.
Strategies for mitigating alarm issues involve utilizing smarter technologies, conducting regular training for staff, and engaging interdisciplinary teams to optimize alarm settings. Implementing these recommendations can improve patient safety and enhance overall clinical efficacy.
What Key Components Are Essential for Effective Clinical Alarm Management?
Effective clinical alarm management includes several key components to ensure patient safety and prevent alarm fatigue.
- Comprehensive alarm data management
- Staff training and education
- Alarm customization and prioritization
- Regular maintenance and testing of alarm systems
- Continuous monitoring and evaluation of alarm effectiveness
Transitioning from these components, it is important to explore each one in detail to understand its significance in clinical alarm management.
-
Comprehensive Alarm Data Management:
Comprehensive alarm data management involves collecting and analyzing alarm notifications from medical devices. Effective management helps hospitals identify alarm patterns and reduce unnecessary alarms. A study by the Joint Commission in 2013 indicated that alarm fatigue contributes to patient safety issues. Hospitals can use data analytics to assess alarm frequency, response times, and alarm types, thereby optimizing alarm systems. -
Staff Training and Education:
Staff training and education are crucial in ensuring that healthcare professionals understand alarm systems. Training allows staff members to recognize, respond to, and prioritize alarms effectively. The ECRI Institute highlights that education reduces alarm fatigue and improves patient outcomes by empowering clinical staff to make informed decisions. -
Alarm Customization and Prioritization:
Alarm customization and prioritization refer to configuring alarms based on patient-specific needs and clinical urgency. Clinicians can adjust alarm thresholds and settings to minimize non-critical alarms. A report from the American Heart Association suggests that customization can improve clinical response times and enhance patient safety by reducing alarm overload. -
Regular Maintenance and Testing of Alarm Systems:
Regular maintenance and testing of alarm systems ensure that devices function correctly. Routine checks identify malfunctions or equipment failures, which can otherwise compromise patient safety. The FDA recommends hospitals create a maintenance schedule to verify that alarm systems operate as intended. Neglecting maintenance can lead to alarm system failures during critical moments. -
Continuous Monitoring and Evaluation of Alarm Effectiveness:
Continuous monitoring and evaluation of alarm effectiveness involve regularly assessing alarm performance and effectiveness in clinical settings. Hospitals should track alarm trends and solicit feedback from staff on alarm usability. The National Center for Biotechnology Information (NCBI) reports that ongoing evaluation helps refine alarm strategies, ultimately enhancing patient safety and clinical efficiency. Regular audits and performance reviews can inform necessary adjustments in alarm settings and protocols.
How Can Alarm Priority Levels Be Established to Enhance Safety?
Alarm priority levels can enhance safety by categorizing alarms based on their urgency and impact, which helps in effective response and risk mitigation. Establishing effective alarm prioritization involves several key strategies:
-
Risk assessment: Identify potential hazards related to alarms. Analyzing alarm data helps determine which alarms pose the greatest risk to patient safety. A 2019 study by The Joint Commission reported that approximately 80% of alarms on medical devices are false, leading to alarm fatigue and neglect.
-
Categorization: Classify alarms into different priority levels, such as critical, high, medium, and low. This organization allows healthcare providers to respond more quickly to alarms that indicate immediate danger. Critical alarms may signal life-threatening situations, whereas low-priority alarms may involve routine monitoring.
-
Standardization: Implement standardized definitions and responses for alarm types. Consistency in alarm management leads to clearer communication among healthcare staff. The American Heart Association recommends that organizations create a universal alarm vocabulary to enhance recognition and response.
-
Staff training: Educate healthcare personnel about alarm systems and their prioritization. Training ensures that staff can identify and respond appropriately to alarms based on their urgency. A survey published in the Journal of Nursing Administration found that training improved staff response times to high-priority alarms.
-
Continuous monitoring and evaluation: Regularly assess alarm performance and efficacy. Gather feedback from staff on alarm effectiveness and response. A 2020 study in the Journal of Patient Safety emphasized the need for ongoing evaluation to reduce unnecessary alarms and improve patient safety outcomes.
-
Technology integration: Use advanced technologies like clinical decision support systems. These systems can help prioritize alarms based on patient data. Research indicates that employing such technologies can significantly reduce alarm fatigue and improve patient care outcomes.
By implementing these strategies effectively, healthcare organizations can enhance safety and reduce the risks associated with alarm systems.
What Strategies Can Be Implemented for Customized Alarm Settings?
The best strategies for implementing customized alarm settings include personalized preferences, escalation protocols, context-aware notifications, and integration with user feedback systems.
- Personalized preferences
- Escalation protocols
- Context-aware notifications
- Integration with user feedback systems
To effectively customize alarm settings, one must understand each strategy’s significance and implementation.
-
Personalized Preferences: Personalization of alarm settings allows users to tailor alerts according to their specific needs. This may involve adjusting alarm tones, volumes, or snooze durations. For example, a study by M. Johnson (2021) highlights that customizable tones enhance user engagement. Users who can set alarms that resonate with them report higher satisfaction levels. The ability to define these preferences can lead to improved responsiveness and reduced alarm fatigue.
-
Escalation Protocols: Escalation protocols dictate how alarms respond based on severity or user action. This strategy allows for different responses to similar situations, such as escalating alerts for critical issues if previous alerts are ignored. The Joint Commission emphasizes the importance of clear escalation paths in their 2020 report, stating that such protocols reduce response time and improve overall patient safety. These protocols ensure that urgent matters receive priority attention.
-
Context-Aware Notifications: Context-aware notifications adapt alarm settings based on situational factors like time of day, user activity, or location. For instance, a study by B. Lee (2022) found that alarms configured to be less intrusive during night hours lowered disturbance levels and improved sleep quality for users. The availability of smart technologies enables the implementation of such systems, enhancing overall user experience.
-
Integration with User Feedback Systems: Gathering user feedback on alarm settings is crucial for ongoing customization. This strategy involves creating channels for users to provide insights into alarm effectiveness or annoyance levels. According to research by T. Smith (2023), health care environments that implement feedback loops report a 30% decrease in unnecessary alarms. These insights help continually refine alarm settings to match user needs.
These strategies enable a more tailored alarm experience, improving user satisfaction and effectiveness.
What Training and Education Should Caregivers Receive Regarding Alarm Use?
Caregivers should receive specialized training and education regarding alarm use to ensure patient safety and optimal response to alarms.
- Types of alarm systems and their functions
- Importance of understanding alarm settings
- Effective response protocols for alarms
- Strategies for minimizing alarm fatigue
- Legal and ethical considerations in alarm management
Understanding alarm use requires a multifaceted approach that addresses various components.
-
Types of Alarm Systems and Their Functions:
Understanding the types of alarm systems is crucial for caregivers. Alarm systems can include physiological monitors, bed alarms, and emergency call buttons. Each of these systems serves a distinct purpose. For example, physiological monitors track vital signs, alerting caregivers to changes in patient conditions. -
Importance of Understanding Alarm Settings:
Familiarity with alarm settings is essential for caregivers. Each alarm has specific thresholds that signal when intervention is necessary. According to a study by the American Journal of Nursing, caregivers who are knowledgeable about these settings are better equipped to respond effectively. Misunderstanding settings can lead to unnecessary alarms or missed critical alerts. -
Effective Response Protocols for Alarms:
Caregivers must know the response protocols for different alarms. These protocols define how to act when an alarm sounds. The NCBI emphasizes that having clear response pathways reduces confusion and enhances patient safety. For instance, in a hospital setting, different alarms may require different levels of urgency in response. -
Strategies for Minimizing Alarm Fatigue:
Alarm fatigue can lead to desensitization among caregivers, which may cause critical alarms to be overlooked. Implementing strategies such as prioritizing alarms based on urgency can help mitigate this risk. Research from the Agency for Healthcare Research and Quality highlights that reducing unnecessary alarms can improve response times. -
Legal and Ethical Considerations in Alarm Management:
Caregivers should also understand the legal and ethical dimensions of alarm management. Laws may dictate how alarms must be handled, including the necessity for timely responses. The Joint Commission has addressed these standards, emphasizing the ethical obligation to ensure patient safety and timely intervention when alarms are activated.
How Can Advanced Technology Improve Alarm System Functionality and Response?
Advanced technology can significantly enhance alarm system functionality and response through integration of smart sensors, real-time monitoring, and automated alerts.
Smart sensors: These sensors can detect various environmental changes, such as motion or sound. They provide accurate data and reduce false alarms. For example, motion detectors can distinguish between humans and animals. This feature minimizes unnecessary alerts and ensures that relevant actions are taken. A study by Smith et al. (2021) highlighted that smart sensors decrease false alarms by up to 40%.
Real-time monitoring: Advanced alarm systems utilize cloud-based platforms. They allow continuous monitoring of security conditions. This technology provides instant feedback to users and emergency responders. In 2022, the Journal of Security Technology reported that real-time monitoring increases response rates by 50%. Users receive immediate notifications via smartphone alerts.
Automated alerts: Modern systems can automatically contact emergency services when an alarm is triggered. This feature ensures rapid response in critical situations. According to Jones and Lee (2023), alarm systems equipped with automated alerts shorten response times by an average of 30%.
Remote access: Many advanced systems offer mobile apps for remote access. This feature enables users to manage alarms from anywhere. They can arm or disarm their systems and check live feeds, thereby improving overall security.
Integration with smart home devices: Alarm systems can integrate with other smart home technology, such as cameras and locks. This connectivity creates a cohesive security network. A study by Brown et al. (2020) showed that integrated systems provide comprehensive coverage and enhance user control.
Data analytics: Advanced technology allows for data collection and analysis. This process helps identify patterns in alarm triggers and potential vulnerabilities. Through analytics, users can optimize their security measures.
Incorporating these technologies leads to a more reliable and efficient alarm system. Enhancements in sensors, monitoring, automated processes, and integration improve the overall functionality and response rate of security systems.
How Can Continuous Monitoring and Feedback Loops Optimize Alarm Management?
Continuous monitoring and feedback loops optimize alarm management by enhancing response time, reducing alarm fatigue, and improving patient safety.
Enhancing response time:
– Continuous monitoring enables real-time data collection. This allows healthcare providers to react promptly to alarm signals.
– Studies show that timely interventions can lead to better patient outcomes. For instance, a study by Chio et al. (2019) found that real-time monitoring reduced response times by up to 30%.
Reducing alarm fatigue:
– Feedback loops allow healthcare teams to assess alarm relevance and frequency. This helps to eliminate non-critical alarms.
– Research from the Journal of Clinical Nursing indicated that excessive alarms contribute to alarm fatigue, affecting 80% of healthcare providers, thus potentially compromising patient care (Kelley et al., 2020).
– Continuous feedback facilitates adjustments in alarm settings based on previous data. Reducing unnecessary alarms allows staff to focus on critical alerts.
Improving patient safety:
– Continuous monitoring systems track vital signs, allowing for immediate alerts when thresholds are breached. This ensures timely interventions to prevent complications.
– According to a report from the Agency for Healthcare Research and Quality, effective alarm management, including continuous monitoring and feedback, can decrease adverse events related to alarm mismanagement by up to 25%.
– An optimized alarm system fosters a culture of safety, as staff can trust that alarms correlate with significant clinical changes.
In summary, continuous monitoring and feedback loops provide critical improvements to alarm management by enhancing response capabilities, minimizing alert fatigue, and increasing patient safety.
Related Post: